Dental implants can be a long-term fix, but paying for them in Texas often feels like decoding two different rulebooks. The CDC reports that 1 in 5 adults ages 20–64 has at least one untreated cavity, and tooth loss is widespread.
An estimate from the American College of Prosthodontists puts it at about 178 million Americans missing at least one tooth. So it’s no surprise most Katy patients ask: Does medical insurance cover dental implants?
In this blog, we will explain medical vs dental coverage, when “medically necessary” cases may qualify, and how to avoid surprises with pre-authorizations and codes.
Start with a Dentist in Katy, TX, for an evaluation to clearly map out costs before you commit.
Key Takeaways
- Dental insurance usually pays for implants, not medical insurance.
- Medical insurance may only cover injury- or health-related cases.
- Most plans do not cover the full cost of an implant.
- Always check your policy before starting treatment.
- Pre-approval helps avoid surprise bills.
- Some claims get denied, but can be appealed.
- Payment options like EMI, HSA, or savings can help.
- Planning early makes treatment easier and less stressful.
Table of Contents
Medical vs Dental Insurance: Who Pays for What?

Dental insurance is usually tied to teeth and gums, while medical insurance is tied to overall health conditions, trauma, and medically necessary treatment.
Quick rule-of-thumb table
| Scenario | More likely billed to | Why? |
| Missing tooth replacement for chewing/smile. | Dental insurance. | Considered a dental restorative service. |
| Tooth loss from accident/trauma (ER, facial injury). | Medical insurance may help. | Injury-related, may involve medical diagnosis codes. |
| Infection, cyst/tumor, jaw surgery, hospital-based care. | Medical insurance may help. | Linked to illness/surgery and medical necessity. |
| Implant crown/abutment for restoring the tooth. | Dental insurance (if covered). | Often treated as a dental prosthetic component. |
What to do before you assume coverage?
Check your plan’s implant wording and limits on the Dental Insurance Plan, then bring your policy details to your consult so the office can verify benefits accurately for your case.
Also Read: Is Dental Insurance Worth It?
When Medical Insurance May Help With Implants in Texas (Injuries, Illness, and “Medically Necessary” Cases)
@charmdentalcare ALL-ON-X vs. Traditional Implants: See how ALL-ON-X provides a faster, more efficient way to replace all your teeth with fewer implants compared to the traditional method⭐️🦷 Here at Charm Dental Care, we’ve got you covered with a brighter smile! 😁 📲 MESSAGE us or tap the link 🔗 in our profile to schedule an appointment. 📍We are located in Katy, Humble, Richmond, and Spring. 💰Financing available #charmdentalcare #houstondentist #topdentist #houstontexas #allonx #dentista #dentistlife #dentist
♬ Raspberry Paradise – Prod. By Rose
Medical insurance doesn’t usually pay for “routine tooth replacement,” but it can help in specific situations where implants are connected to a medical diagnosis, trauma, or surgical treatment plan.
This is where the phrase medically necessary dental implants comes in.
Situations where medical insurance may contribute
1. Injury or accident-related tooth loss
If a tooth is lost due to facial trauma (sports injury, fall, auto accident), some aspects of care may be processed under medical coverage.
2. Disease, pathology, or surgical treatment
When implants are used to treat an infection, a cyst, a tumor, or to perform jaw surgery or reconstruction, medical insurance may cover certain steps (especially the hospital/surgical portions).
3. Congenital conditions or medically complex cases
Some plans consider coverage when tooth absence or jaw issues are part of a broader medical condition that requires functional rehabilitation.
Charm Dental Care Katy
What medical may cover vs what it usually won’t
- May help with: diagnostics (imaging), surgical portions, hospital or anesthesia components (case-dependent).
- Usually won’t cover: the implant crown/abutment as a standard “tooth replacement” benefit.
Why documentation matters?
Medical insurers typically want:
- a clear diagnosis and narrative of medical necessity,
- treatment notes explaining function (chewing, speech) and health impact,
- codes that match the diagnosis and procedure pathway.
If you want to see who evaluates these cases and how treatment planning is handled, take a quick look at our professional Dentists before your consultation, so you know the team guiding your implant and coverage approach.

What Typical Dental Plans Cover (and Don’t Cover) for Implants
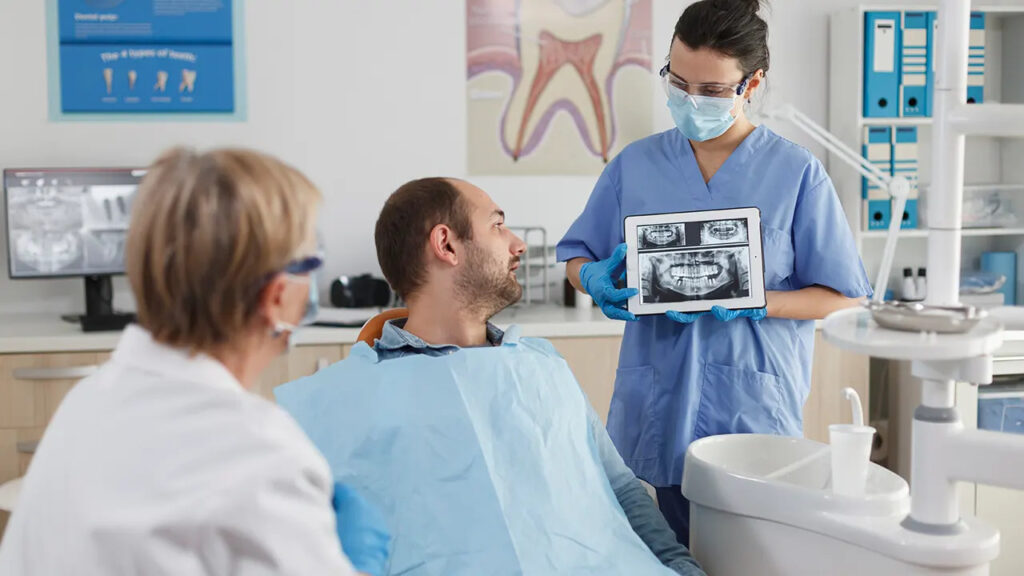
Most plans treat implants as a “major” service, which means limits, waiting periods, and exclusions are common.
When people ask about dental implant insurance coverage, the real answer is usually: some parts may be covered, but rarely all of it.
What dental plans may cover (often with limits)?
- Implant crown (the visible tooth on top), sometimes categorized as a major restorative.
- Implant components in certain plans (varies a lot).
- Related services like exams, X-rays, and teeth cleanings (under preventive).
- Bone grafting or extractions are sometimes, but often with strict rules.
What dental plans often don’t cover?
- Full implant fees with no cap (many plans have annual maximums).
- “Missing tooth clause” limitations (if the tooth was missing before coverage started).
- Upgrades, premium materials, or extra cosmetic work.
- Parts of treatment if you’re out-of-network (depending on plan type).
@charmdentalcare Wanted to show her ex the new smile… But we don’t allow toxic calls in this clean space.#Smile #dentist #CharmDental #dentista #dentist #dentalcare #houstondentist #funny
♬ Welp, Didn’t Expect That – Yu-Peng Chen & HOYO-MiX
Fast coverage-check table
| Item to check | Why does it matter? |
| Annual maximum | May cap benefits even if implants are “covered.” |
| Waiting periods | Some plans delay major service coverage. |
| Missing tooth clause | Can block implant coverage for pre-existing missing teeth. |
| In-network rules | PPO vs DMO can change provider choice and pricing. |
| Implant exclusions | Some plans exclude implants but cover bridges/dentures. |
At Charm Dental Care, you’ll find the clinic’s patient-first approach helpful, as implant planning is not just clinical; it’s also about setting realistic expectations for the timeline and payment from day one.
Also Read: Dental Insurance Financing at Charm Dental
Pre-Authorizations, Codes and “Fine Print”: How to Read Your Policy Before You Start Treatment

Before you schedule anything major, slow down and check whether your plan requires a pre-authorization from your dental insurance. This one step is where most “surprise bills” come from.
Step 1. Find the 3 lines that control your implant benefits
- Is implants coverage listed at all (or excluded).
- Annual maximum (your true cap for the year).
- Waiting period + missing tooth clause (the two most common blockers).
Step 2. Ask for the exact codes before you commit
You’ll usually need codes for:
- implant placement
- abutment
- Dental crown
- bone graft (if needed)
- extraction (if needed)
- imaging (CBCT or X-rays)
Step 3. Check the “fine print” that changes the final number
- In-network vs out-of-network rules.
- Percentage coverage for “major services.”
- Frequency limits (how often certain items are allowed).
- Whether anesthesia/sedation is covered separately.
A simple way to avoid back-and-forth
If you want help gathering the right details to submit, Contact Charm Dental Care and ask what info they need to run a benefits check and whether your plan requires pre-approval before implant treatment starts.
Also Read: Are Dental Expenses Tax Deductible?
Texas-Specific Considerations: Employers, PPOs, DMOs, and Medicaid Limits
@charmdentalcare 🚨ATTENTION HOUSTON🚨We are hosting a FREE Dentistry Day! 🌟Services: Enjoy FREE cleanings, exams, fillings, implants, root canals, crowns, extractions, and emergency care (one procedure per person, first come first serve). ⏰Date & Time: Saturday, June 1st, from 8:30 am to 3 pm. 📍Location: Charm Dental Care RICHMOND Address: 2201 Thompson Rd 101, Richmond, TX 77469. HOW TO PRE REGISTER: Secure your spot via the top 🔗 in our profile **Minors must be accompanied by a legal guardian. Priority for veterans, pregnant women, and those in pain. #freedentistryday #charmdentalcare #dentistinhouston #houstondentist #katydentist #houston #houstontx #dentalcare #hosuton #veneers #crowns #implants #dentures #braces #invisalign #extractions #rootcanals #dentalassistant #dentalcare
♬ My Girl Wukileak – wüki
Implant coverage in Texas isn’t one standard rule; it changes based on whether you’re on an employer plan, a PPO, a DMO, or Medicaid.
That’s why “Texas rules” often feel inconsistent, even when two patients live in the same city.
1. Employer plans (Texas reality)
Many Texans get dental coverage through their employers, but implant benefits can vary widely depending on plan design. Some cover implants as a major service, while others exclude implants but cover bridges or dentures.
2. PPO vs DMO (why it matters)?
PPO plans
- More provider flexibility (you can usually choose your dentist).
- Coverage is often percentage-based, with annual maximums.
DMO plans
- Lower upfront fees but stricter network rules.
- Often, limited provider choice and preset copays (with implants possibly restricted).
3. Medicaid limits
Texas Medicaid dental benefits depend on eligibility category and age, and adult coverage can be more limited than for children.
Even when dental benefits exist, implants are not typically covered unless there’s a specific medical condition.
Charm Dental Care Humble
If you’re comparing coverage across nearby areas, it can help to see how benefits questions are handled at different clinics that many patients book across locations, like a dentist in Humble, TX, when checking availability and insurance timing.

How to Call Your Insurance and Get Straight Answers About Implant Coverage?

Insurance reps can be vague unless you ask very specifically. Use this script so you don’t get a “maybe” answer.
This also helps if you’re learning how to read dental insurance language in real time.
The 7 questions to ask
- “Does my plan cover dental implants at all, or are implants excluded?”
- “If implants are covered, are they covered under major services, prosthodontics, or a separate implant benefit?”
- “What is my annual maximum, and how much of it is remaining this year?”
- “Is there a waiting period for implants or major services?”
- “Is there a missing tooth clause, and does it apply if the tooth was missing before my coverage started?”
- “Do I need pre-authorization before implant placement, abutment, or crown?”
- “Is my provider in-network, and how does out-of-network reimbursement work if not?”
What to request before you hang up?
- Reference number for the call.
- Rep’s name/ID.
- A copy of the benefits emailed to you (or a link to the policy PDF).
Charm Dental Care Spring
If you want the fastest path to verification, many patients schedule benefits checks based on availability, sometimes even checking nearby locations, like a dentist in Spring, TX, while coordinating timing for consults and insurance windows.
If Your Claim Is Denied: Appeal Letters, Extra Documentation, and When to Try Again
A denial isn’t always the final answer; often it’s a paperwork problem, a coding mismatch, or missing documentation.
If you’re dealing with an implant denial, the right approach is an organized appeal to the dental insurance denial process.
The most common denial reasons
| Denial reason | What it usually means | What to submit next |
| “Not medically necessary.” | They don’t see health/functional need. | Letter of medical necessity + diagnosis support. |
| “Implants excluded.” | Plan language blocks implants. | Ask if any related services are covered (extractions, grafts, anesthesia). |
| “Missing tooth clause.” | Tooth missing before coverage date. | Provide dates, records, and ask for exception review (rare, but possible). |
| “No pre-authorization.” | Approval was required first. | Retro-auth request + clinical notes (may or may not be accepted). |
| “Out of network.” | Coverage reduced or denied under network rules. | In-network option review + reimbursement details. |
What strengthens an appeal?
- Clinical notes explaining functional impact (chewing, pain, infection risk).
- X-rays/CBCT findings.
- Photos and periodontal charting when relevant.
- Medical history tie-in (trauma, pathology, surgery, disease-related loss).
- A short, clear appeal letter that matches the insurer’s denial language.
When it’s smart to re-submit vs move on
- Resubmit if the denial is missing documents, contains incorrect codes, or lacks a narrative.
- Move on if implants are clearly excluded and there’s no exception pathway.
Charm Dental Care Richmond
If you’re coordinating care and documentation across different offices, patients sometimes choose whichever clinic location has the soonest consult window, like Dentist in Richmond TX so records and insurance follow-ups don’t drag out for weeks.
When Insurance Won’t Help: HSAs, FSAs, Discount Plans, and In-House Financing

If your plan excludes implants or the benefits cap is too low, you still have options.
The goal is to build a plan that matches your timeline and cash flow, especially if you’re exploring dental implant financing options.
Option 1. HSA or FSA (often the cleanest way)
- HSAs/FSAs can usually be used for qualified dental expenses.
- If you’re eligible, using pre-tax dollars can reduce the real “out of pocket” hit.
- Keep receipts and treatment plans for documentation.
Option 2. Discount plans or membership-style savings
- These aren’t insurance policies, but they can reduce prices for certain services.
- Great if you don’t have dental insurance and want predictable savings.
Option 3. In-house financing or monthly payments
- Helpful for spreading the cost over time instead of paying all at once.
- Ask what’s included and whether payments cover all phases (surgery + crown).
If monthly budgeting is the key for you, the easiest place to start is Flexible Dental Payment Options, which outlines how patients can break treatment into manageable payments.
Using Your Tax Refund Wisely: Spreading Out Big Implant Cases Over Time

A tax refund can be a smart “jump start” for implants, especially if you’re planning a multi-step case.
Many patients use it to cover the first phase, then spread the rest out through savings, monthly payments, or an HSA for dental implants strategies if they’re eligible.
If you don’t have dental coverage and want predictable pricing support as you plan, the Dental Membership Plan may be worth reviewing early so you know what ongoing care might look like.
A practical way to split implant treatment
Phase 1. Evaluation + imaging
Use your refund to cover diagnostics and planning so you know the true total early.
Phase 2. Surgical phase (extraction/graft/implant placement if needed)
This is often the biggest step. Some patients pay part upfront and finance the remainder.
Phase 3. Healing phase (time buffer)
Healing time can give you weeks or months to rebuild savings before the final tooth is placed.
Phase 4. Final restoration (abutment + crown)
Plan for this as a separate expense if your benefits reset annually.
Why does this approach work?
- You avoid trying to fund everything in one month.
- You can time phases around annual insurance maximums if dental benefits apply.
- You reduce financial stress while still moving forward.
Simple Checklist to Bring to Your Katy Implant Consultation

Walking into your visit prepared saves time and prevents “I’ll call you back” insurance answers. Use this checklist of questions to ask the dental implant dentist, and bring the right documents so the estimate is accurate.
Bring these documents
- Your insurance card(s): dental + medical (if you have both).
- Member ID, group number, and employer plan name.
- Any denial letters or prior authorization notes (if you already tried).
- A list of medications and relevant medical history (diabetes, smoking, bone meds, etc.).
Ask these questions
- Is my case likely dental-only, or could medical insurance apply?
- What codes will be submitted for my implant plan?
- Do I need pre-authorization before anything starts?
- What is included in the estimate (imaging, graft, implant, abutment, crown)?
- Can treatment be phased across benefit years to reduce out-of-pocket.
- What financing or payment plan choices do I have if coverage is limited?
If you want a quick visual feel for outcomes and smile restoration work, our Dental Clinic Gallery will help you prepare questions, so you know what results you’re aiming for and what to ask about.

Why Choose Charm Dental Care for Your Dental Implants in Katy?
Implants are both a clinical and financial decision, so it helps to work with a team that keeps the process clear from the first visit.
1. Clear, step-by-step planning
At CharmDental Care, you’ll see a patient-first approach that focuses on explaining treatment stages, timelines, and what to expect, especially helpful when implants are spread out over multiple phases.
2. Insurance-friendly support and practical payment options.
Because coverage rules can be confusing, patients often ask for help verifying benefits and understanding what’s included before treatment starts. If insurance won’t cover enough, Flexible Dental Payment Options make it easier to plan monthly costs without delaying care.
@charmdentalcare At Charm Dental Care, we’ve got you covered with our financing options! ⬇️ 💰Care credit 💰Sunbit 🍒Cherry payment plans To apply or learn more about our payment plans, tap the 🔗 in our profile or MESSAGE US. 📍We are located in Katy, Richmond, Spring, and Humble #charmdentalcare #paymentplans #houstondentist #cherrypaymentplans #besthoustondentist #veneers #crowns #smilegoals #dentalcare
♬ Money In The Summer – Brentin Davis
3. Convenient next step in Katy
If you’re ready for clear answers, the simplest move is to book a Dental Appointment for a consultation and request an implant cost estimate with an insurance check.
You Might Also Like
- How Much Does a Single Tooth Implant Cost in Katy, TX (2026 Pricing Guide)
- Full Mouth Dental Implants Cost
- The Patient’s Guide to Dental Implant Surgery
Building a Realistic Payment Plan You Can Stick To
Implants are a big decision, and the smartest way to pay is the way that keeps you consistent, no panic, no surprises, and no half-finished treatment. Start by confirming whether your case could qualify under medical (trauma, illness, medically necessary situations), then check what your dental plan actually covers and where the annual maximum caps your benefit.
If you want to reduce stress, break the case into phases, line up pre-authorization early, and use tools like HSAs/FSAs, discount plans, or monthly payments when insurance falls short. If timing matters, it can also help to visit Current Dental Offers and plan your consult around coverage windows.
FAQs (Frequently Asked Questions)
Q1. Will My Medical Insurance Pay For Dental Implants?
Sometimes, but not for routine tooth replacement. Medical insurance is more likely to cover implant-related care when it is tied to a medical condition, trauma, surgery, or a “medically necessary” diagnosis pathway. Most standard implant placement and crowns are still processed either under dental benefits or out of pocket.
Q2. What Is The Difference Between Medical And Dental Insurance For Implants?
Medical insurance typically covers health-related diagnoses (injury, illness, surgery, hospitalization, or anesthesia). Dental insurance focuses on teeth and restorative services, and may cover parts of implant treatment depending on exclusions, annual maximums, and plan rules.
Q3. In What Situations Will Medical Insurance Cover Implants?
Medicine may contribute when tooth loss is linked to facial trauma, disease/pathology (cyst, tumor removal), jaw reconstruction, or medically necessary treatment planning. Coverage often applies to diagnostics or surgical components, not always the implant crown or final tooth restoration.
Q4. How Much Will My Dental Plan Cover For Implants?
It varies a lot. Many plans treat implants as a major service with percentage coverage and an annual maximum that caps how much the plan will pay in a year. Some plans exclude implants entirely or limit coverage due to waiting periods or missing-tooth clauses.
Q5. Do I Need Pre-Approval Before Getting Implants?
Many plans require pre-authorization (or strongly recommend it) for major services like implants. Getting pre-approval helps prevent denials based on missing paperwork, incorrect coding, or “not authorized” technicalities.
Q6. Does Medicaid Or State Insurance Cover Dental Implants In Texas?
Texas Medicaid dental benefits depend on eligibility and age. Adult dental coverage can be limited, and implants are rarely covered, except in rare, medically complex situations. The best step is to confirm your exact plan benefits and limitations directly with your insurer.
Q7. What Should I Ask My Insurance About Implants?
Ask if implants are covered or excluded, whether a missing-tooth clause applies, what your annual maximum is, whether pre-authorization is required, and how in-network vs out-of-network rules affect your total cost.
Q8. What Can I Do If My Implant Claim Is Denied?
Start by reading the denial reason carefully. Many denials can be appealed with better documentation, corrected codes, supporting imaging, and a brief letter explaining medical or functional necessity. If implants are clearly excluded, you can ask if any related services (extractions, grafting, anesthesia) are covered.
Q9. What Are My Options If Insurance Won’t Pay For Implants?
You can consider monthly payment plans, discount- or membership-style savings, or phasing treatment over time to spread out costs. Many patients also use HSAs/FSAs when eligible, which can reduce out-of-pocket costs.
Q10. Can I Use HSA Or FSA For Dental Implants?
In many cases, yes, HSAs and FSAs can often be used for qualified dental expenses, including implants. Keep your receipts, treatment plan, and itemized statements for documentation and reimbursement purposes.
Q11. What Should I Ask Before Starting Implant Treatment?
Ask what’s included in your estimate (implant, abutment, crown, imaging, bone grafts, follow-ups), what codes will be submitted to insurance, whether pre-authorization is needed, and whether your case can be phased across benefit years to reduce costs.


























